Introduction
The reported prevalence rate of female sexual dysfunction (FSD) varies widely from 19% to 45% depending on the definition of FSD used and the age groups reported (1-4). Evaluation of sexual dysfunction greatly depends on patient self-reporting.
A variety of assessment tools are currently available to help screen and assess FSD. Among these, the Female Sexual Function Index (FSFI) is the most widely used questionnaire (5). The FSFI consists of 19 items distributed across 6 domains, including desire, arousal, lubrication, orgasm, satisfaction, and pain. The FSFI-19 has been translated into Korean, and its reliability and validity have been verified (6). Although it is one of the most useful and meaningful assessment tools for the diagnosis and treatment of FSD, patients may feel uncomfortable and reluctant to complete the 19-item-long questionnaire in public (7-9). To address the issue of length, Isidori et al developed the FSFI-6, which simplified the FSFI by including a single question for each of the six domains (10). Naturally, the FSFI-6 offers the advantages of conciseness and speed (requiring less than 3 minutes to complete).
Because each domain of FSD has various symptoms with complex pathogenesis, the larger disorder category was recently divided into female sexual interest/arousal disorder, female orgasmic disorder, and genito-pelvic pain/penetration disorder (11-14).
In the current study, we selected five of the six domains in the FSFI (desire, arousal, lubrication, orgasm, and satisfaction), excluding the pain domain, to develop and validate the FSFI-5 as a rapid screening tool for female sexual disorder.
Materials and Methods
We interviewed and administered the FSFI-19 and FSFI-5 questionnaires to healthy volunteer women. A total of 220 married women were recruited to participate in the study. The inclusion criteria required that volunteers agree to complete all questionnaires, have no active infection, and have been in a stable sexual relationship with a male partner for at least the past 6 months.
Initially, all subjects completed the full-length FSFI-19 and the FSFI-5. According to the international cutoff value, participants with an FSFI-19 score <26.55 were classified in the “female sexual dysfunction” group. After 3 weeks, all participants were asked to complete the FSFI-5 and FSFI-19, respectively. This study was approved by IRB of the Chonnam National University Hospital (CNUH-2013-154).
We excluded the “pain” domain from the FSFI-19 and made the FSFI-5, which consisted of item-by-item combinations of the five domains of sexual “desire”, “arousal”, “lubrication”, “orgasm”, and “satisfaction”. Representative items of each domain were selected from the FSFI-19 by referring to the FSFI-6 (Appendix 1).
PASW Statistics for Windows, version 18.0 was used to assess the validity of the FSFI-5. Basic data were obtained by using mean values ± standard deviations. Receiver operating characteristic (ROC) analysis was performed, and Cronbach’s alpha was calculated to verify the internal consistency of the tool. To obtain the test-retest reliability of the two questionnaires, the Pearson correlation coefficient was calculated by using the results of two rounds of questionnaires. For validity analysis, a cutoff score was obtained with optimal sensitivity and specificity required to screen individuals with sexual dysfunction.
Results
Of the initial 220 participants, 197 were finally enrolled in this study. Three women (1.4%) did not complete the questionnaires and were excluded from the study population. Twenty women (9.1%) were eliminated for having no sexual activity during the previous 4 weeks.
Table 1 shows the characteristics of the study population. The mean age of the enrolled volunteers was 35.93 ± 4.26 years (range: 25 to 50 years) and the mean body mass index (BMI) was 21.15 ± 2.04 kg/m2. A total of 5 women (2.5%) had hypertension, 3 (1.5%) had diabetes mellitus, 10 (5.1%) had a personal history of reproductive system diseases (uterus, ovaries, etc), and 4 (2.0%) were current smokers.
Of the 197 final participants, 89 with an FSFI-19 score <26.55 points were classified into the FSD group. In the comparison of clinical factors between the FSD and non-FSD groups, age (p=0.317), BMI (p=0.220), and marriage duration (p=0.132) showed no significant differences, whereas the participants with FSD had a lower intercourse number during the previous 4 weeks (4.84 ± 1.31 vs 6.30 ± 1.78, p<0.001) (Table 2).
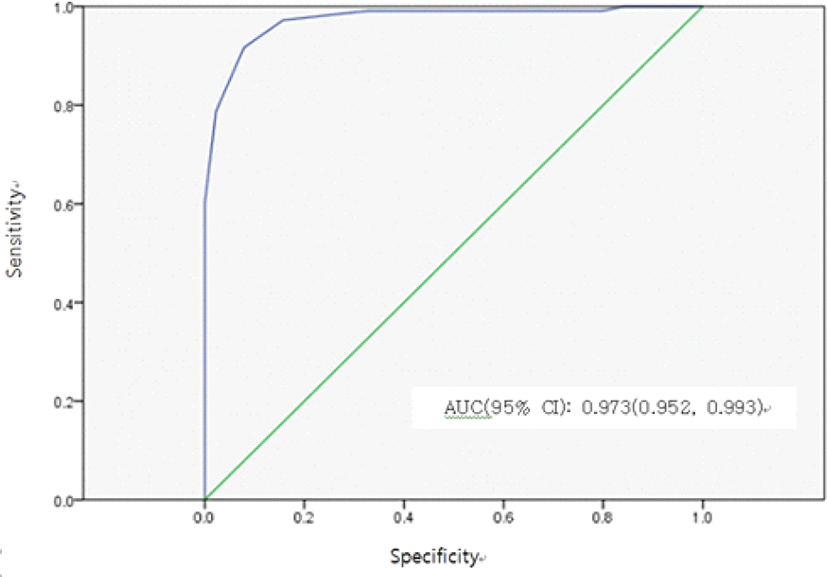
The score for each item on the FSFI-5 and the total score of the FSFI-5 were significantly lower in the FSD group than in the non-FSD group (p<0.001, Table 2). Fig. 1 shows the ROC curve for the FSFI-5. The estimated area under the ROC curve (AUC) was 0.973 (95% confidence interval: 0.952 ~ 0.993). The ROC curve was performed to find the FSFI-5 cutoff value for making a diagnosis of FSD. As shown in Table 3, the sensitivity and specificity of the FSFI-5 were 91.7% and 92.1%, respectively, at a score of 18. Women who scored <18 were diagnosed as having FSD, whereas those who scored ≥18 were diagnosed as not having FSD.
In the analysis of internal consistency of the FSFI-5, the responses for the five domains showed a strong correlation. Cronbach’s alpha was 0.887, suggesting a very high level of reliability, and the Pearson correlation coefficient was 0.707 (Table 4).
DISCUSSION
The FSFI is a self-reported, 19-item questionnaire assessing sexual function. It is one of the best tools for diagnosing FSD and for monitoring treatment (15). Because of its usefulness, the FSFI has been used consistently in outpatient clinics, but is sometimes considered too long for routine use. To reduce patient discomfort and to create a rapid screening test for FSD, Isidori et al (10) developed the FSFI-6, an abridged form of the FSFI.
Although the FSFI-19 has six domains for assessing female sexual dysfunction, sexual pain can be associated with infection or inflammation of the vulva or vagina or can be related to psychosexual disorder. Therefore, the sexual pain domain needs to be evaluated separately for the screening of sexual interest/arousal disorder. In the present study, we designed and validated the Korean version of the FSFI-5 as a rapid screening tool for female sexual dysfunction. Additionally, we determined the cutoff score with optimal sensitivity and specificity.
A questionnaire’s validity consists of item validity, discriminating power, and linguistic validity. Reliability is assessed with the test-retest reliability index and the internal consistency index of each domain. The reliability and validity of the Korean FSFI were tested and proven previously (6). Because the FSFI-5 is a simplified version of the FSFI, additional verification was deemed unnecessary. Additionally, the selection process for optimal items was waived, because the FSFI-5 consists of a single item selected from each domain of the FSFI-6 with exclusion of the “pain” domain.
Of 197 survey participants, 89 were suspected to have female sexual dysfunction, yielding a prevalence rate of 45%. The prevalence rate of FSD in our study was higher than reported in other previous studies (16, 17). In the current study, individuals with FSFI scores of less than 26.55 points were considered to have sexual dysfunction. This reference point was deduced on the basis of a study by Wiegel et al (18). The sensitivity and specificity of the Korean FSFI-5 were assessed on the basis of this reference point, and the optimal cutoff score was suggested on the basis of the ROC curve. Whereas the current study determined an FSFI score of 26.55 to be an acceptable cutoff, a Turkish study by Oksuz et al (19) assessed a prevalence rate using a cutoff score of 25 points. The prevalence rates of the current study and a study by Song et al (17) are similar, at 42.9% and 43.1% respectively. However, Oksuz et al reported a higher prevalence rate of 48.3%. This discrepancy may be due to sociocultural and linguistic differences between the two countries.
In this study, Cronbach’s alpha, which evaluates the internal consistency level of each domain in the female sexual dysfunction questionnaire, was relatively high at 0.887. The intraclass correlation coefficient, which measures test-retest reliability, was also high, at 0.816. However, the Pearson correlation coefficient between the first and second rounds of the survey was 0.707, lower than in previous results. It is also worth noting that most of the eliminated participants reported no sexual activity for 4 weeks in response to one the questionnaires. This implies changes in sexual activity patterns during the 3 weeks between the test and the retest. The same issue has been reported in the other studies, which prompted a modification to the Japanese version from “the past 4 weeks” to “the past 3 months” (20). Nevertheless, the relatively low Pearson correlation coefficient still exceeds 0.7 (a standard required for group questionnaires) (21) and therefore satisfies the original intent of the questionnaire.
The FSFI-6, a simplified version of the FSFI, offers the advantages of convenience and speed because it takes less than 3 minutes to complete (22). The FSFI-5 has the same advantages. The Cronbach’s alpha of the FSFI-5 was 0.887, which is higher than that of the FSFI-6 (10). The reliability of the FSFI-5 was higher than that of the FSFI-6 because the pain domain showed a weak indirect correlation in the FSFI-6. The AUC of the FSFI-5 was 0.973 (0.952-0.993), which did not differ greatly from the AUC of 0.984 (0.951-0.997) of the FSFI-6. A study by Lee et al (11) found the Cronbach’s alpha and AUC of the FSFI-6K to be 0.888 and 0.948 (0.92-0.976), respectively, similar to the results of our study. Therefore, the reliability analysis indicates that the FSFI-5 has sufficient reliability as a tool for screening of FSD.
The current study had limitations. First, the participants were limited to relatively young women residing in the local area. Therefore, the prevalence rate in this study cannot be generalized across the female population in Korea. Second, we did not evaluate the effect of the pain domain. Future study is needed to compare the FSFI-6 and the FSFI-5 in women with FSD.
In conclusion, the current study developed and verified the FSFI-5, which is based on the Korean version of the FSFI. The questionnaire’s internal consistency showed high reliability, and the reliability correlation coefficient was statistically significant. Therefore, the FSFI-5 may be a useful tool to screen Korean women with female sexual disorder. Further research is needed to evaluate the role of the pain domain, which was not included in the FSFI-5.







